Practical Tips for Trying to Conceive with PCOS
Updated November 24, 2025
Polycystic ovary syndrome (PCOS) is one of those conditions known to be difficult to diagnose. The most firm and accurate diagnosis will usually come from blood tests.
The list of symptoms for PCOS is long and includes (but is not limited to):
- Missed and/or irregular periods
- Large ovaries or ovaries with many cysts
- Hirsutism (excessive body hair especially on the chest, stomach and back)
- Obesity
- Anovulatory cycles (no ovulation)
- Infertility
A person may possess all or one of these symptoms, making it difficult to diagnose - especially because some of these symptoms can also be indicative of other issues in your body other than PCOS.
One of the first things many providers tell their patients with PCOS is they will likely have trouble conceiving. Let's look at the reason behind that statement!
How can PCOS impact fertility?
One of the first things many people recognize to make them suspect unregulated PCOS is often long, irregular cycles. This can cause difficulty in achieving pregnancy. For those charting their cycles, it can be common to experience ongoing vaginal discharge and delayed ovulation. It's not uncommon for people with PCOS to experience cycles 40 - even 60 - days in length. In addition, the person may not ovulate every cycle but can continue to experience a bleed, either regularly or irregularly. For those not charting, this breakthrough bleeding can easily be mistaken for true menstruation.
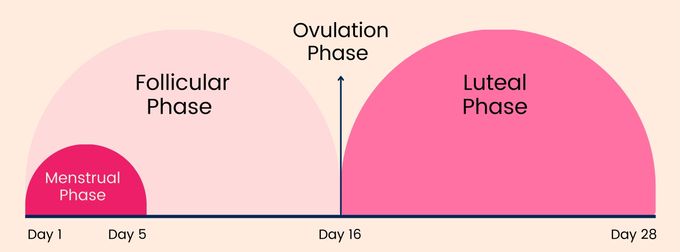
When trying to conceive, most doctors will recommend timing intercourse around day 14 of the cycle, since the textbook assumption is you'll ovulate within a day or two of day 14. However, this assumption is also based on a cycle length of 28 days, which isn't very typical in those with PCOS.
Your luteal phase (the time after ovulation) will remain relatively constant, so those with PCOS would ovulate 8-18 days before their next period is expected. A person with PCOS may not ovulate until day 30 or later with long cycles, and even then unpredictably. So you can see how conception would not occur cycle after cycle if they're timing intercourse for day 14. This may result in a visit to a provider and a recommendation to complete IUI and/or IVF treatments to conceive because of infertility.
Where can you start if you are attempting to conceive?
I recommend you start by tracking their cycles through the fertility awareness method. Because PCOS charting can be tricky, I suggest finding a fertility awareness educator - someone who is certified, and perhaps even specializes or has plenty of experience in working with those who have PCOS.
Tracking your cycle via a fertility awareness method can be invaluable, particularly when you are trying to conceive. If you suspect unconfirmed PCOS, tracking your cycles (menstruation, ovulation and luteal phase) can be a way to gain valuable information that can be used as an aid, and diagnostic tool, to assist your provider in a confirmed diagnosis.
Which method would be valuable for someone with PCOS when they are looking to conceive?
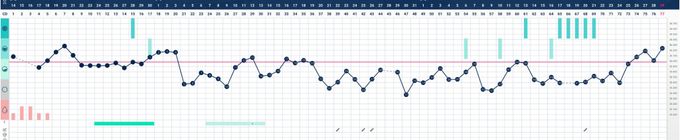
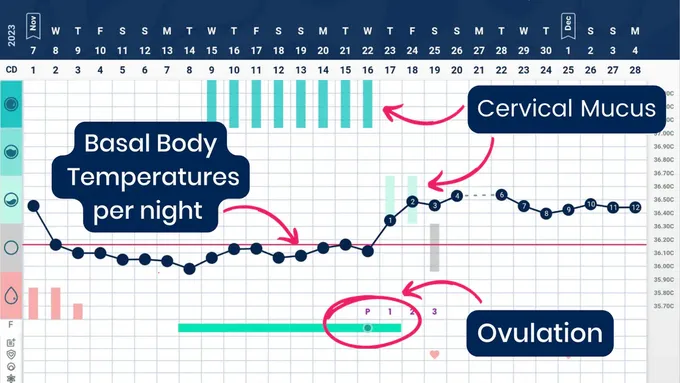
I recommend a method including both cervical mucus and basal body temperature (a Symptothermal method). The method I teach, FEMM, is a great example! The cervical mucus can assist a person in determining periods of fertility, and infertility, through patterns of mucus production. As mentioned above, it's common for someone to experience constant discharge, and in working with an instructor you can determine when you have entered a period of fertility or when the patterns remain infertile.
The second piece is incorporating basal body temperature (BBT). I personally love Tempdrop!
While cervical mucus indicates when you're approaching ovulation, adding BBT gives you a way to confirm ovulation. When someone experiences long, irregular cycles and irregular mucus patterns, utilizing the basal body temperature can assist in confirming when ovulation occurs AND can assist in detecting anovulatory cycles (when ovulation did not occur). Both of these signs of fertility can assist a person in gaining valuable information about their cycles and have the potential to increase your chances of conception by accurately detecting ovulation.
What else to consider with PCOS, while trying to conceive?
I recommend people with PCOS get a complete workup with their care provider, preferably one who is well-versed in a fertility awareness method and PCOS. The FEMM medical management program is a good place to find providers who are familiar with and supportive of fertility awareness.
Additionally, I recommend you see a nutritionist who specializes in PCOS. Since we know dietary changes have the ability to help people with PCOS improve symptoms, make cycles more regular, and generally increase chances of conception.
Finally, I suggest finding a naturopath; once again – someone who is well-versed in hormones and PCOS. Naturopaths have the ability to complete comprehensive lab testing for hormones and aid in improving hormone health through natural means.
For some, a diagnosis with PCOS can seem like a lifetime sentence along with the fear of infertility when the time comes to start a family. Fortunately, there are many options available, and although it may not be easy, there is hope!
Other Tempdrop articles about PCOS
- PCOS GUIDE: How to speak to your doctor
- PCOS Guide for Clinicians
- PCOS: Understand your cycle and how to get pregnant
- What are the benefits of Tracking Ovulation when you have PCOS
- 5 Tips for Tracking Your Cycle When You Have PCOS
- Simple, Effective Nutrition Tips for People with PCOS
- 5 Unusual Signs & Symptoms of PCOS You Should Look Out For
- Food & PCOS: What to Avoid and What to Enjoy Guilt-Free
- Endometriosis vs. PCOS: Understanding the Impact on Fertility
- What is PCOS? Understand hormones, symptoms & get a diagnosis