The Right Way to Talk About Your Cycle
Updated July 7, 2025

Your cycle is shorthand for your “menstrual cycle.” Here’s where some confusion comes in, because your menstrual cycle isn’t exactly the same as your menstrual period. So, let’s start by talking about bleeding!
Your first menses arrives after your first ovulation. Menses is the bleeding that occurs usually 10-16 days after ovulation; it’s what starts the next cycle.
You may use other words for it instead of calling it menses or menstruation or menstrual period: “Aunt Flo(w)” or “AF” for short, “cycle”, “the cavalry”, the “red dawn”, your “monthly”, the “girl flu,” the “curse”, your “womanly time”, “shark week”… I can think of dozens. There are probably hundreds, even thousands of euphemisms for this around the world. There's some common themes, but a wide variety, so collecting these euphemisms can be pretty fun.
One quirk about human societies is that we aren’t always in the habit of using “correct” medical or formal terminology for our bodies. In many ways, that’s fine! We’re not all medical professionals in clinical settings and speaking like one can sure sound weird in casual conversations. But sometimes it causes problems.
Why Does It Matter?
As a Fertility Awareness educator, I spend a lot of time listening to women talk about their reproductive health and intentions, and I’ve noticed that sometimes the terminology used doesn’t fit well with how we usually talk about fertility charting. That’s not always a problem, but sometimes it can point to a lack of knowledge.
Knowledge about our own bodies, in all their wondrous complexity, is essential! Knowledge is power. The knowledge of correct terminology can provide us with the clarity we need to understand a subject, and to convey that information to others (including medical professionals) when needed.
What Is A Cycle?
When I ask women how long their cycles usually are, sometimes I get an answer about how many days their bleeding lasts. These ladies are in the habit of calling their bleeding a “cycle.” The problem is that biologically, and in fertility charting, a cycle and bleeding is not the same thing. A “cycle” is the time from the beginning of your menses, through ovulation, and it finishes the day before your next menses begins. So a cycle is not the menstrual period by itself!
- A cycle starts with menstruation (which usually lasts 3-7 days)
- BUT it doesn’t end when your bleeding goes away. It continues on.
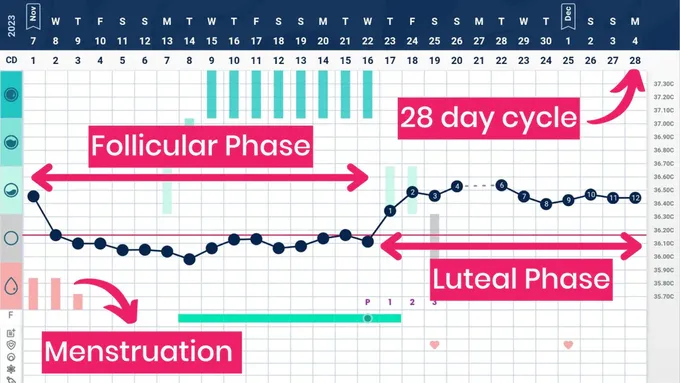
A Tempdrop chart example showing a 28 day cycle with a 3 day period, follicular phase and luteal phase
How Should We Talk About Menstruation?
The word “period” is very commonly used to describe menstruation. It’s a well-accepted word in common usage; my family doctor and nurse practitioner use it to talk with patients. It’s short for “periodic bleeding,” which is what menses is. We can call it your menstrual period!
But many women will describe any bleeding as a period. This can obscure information that could be vital for analyzing your health, trying to conceive, or trying to avoid.
For example, if you get just two days of spotting on cycle days 22 and 23, and nothing after that, that bleeding is not a “period” in the sense that it is almost certainly not menses. That sort of bleeding might happen periodically, but it is not a menstrual period (menses). It could be:
- Ovulation spotting
- Breakthrough estrogen bleeding
- Implantation related bleeding
It’s very unlikely to be a real menses, though.
This has implications for whether you start a new cycle chart, what to do if trying to avoid pregnancy or trying to conceive, along with simply knowing how long your cycles really are, how to communicate that with your healthcare provider, and when you might expect a menses. (That, by the way, has got to be one of my favorite aspects of fertility charting. Knowing reliably within a day or two when to expect menstruation, so I can be prepared.) So, now that we know that your menses alone isn’t a cycle, and we know a cycle extends through menses, ovulation and until the next menses begin, let’s talk about how to divide up the parts of the cycle, and how to refer to these divisions.
How Do We Talk About The Divisions Of A Cycle?
There are a couple of different approaches to this:
- There is the biological division of the cycle
- or the fertility awareness based method (FABM) division of a cycle
Biologically, a cycle could be divided a number of ways:
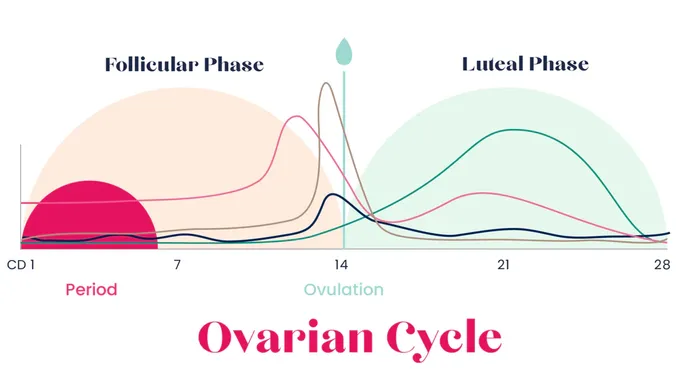
- One common way is to split it in two pieces, with ovulation as the dividing line:
- So you have a pre-ovulation phase called the “follicular” phase,
- a post-ovulation phase called the “luteal” (loo-TEE-uhl) phase.
- Sometimes you may see it divided into three parts instead:
- a menstrual phase covering the bleeding at the beginning of the cycle,
- follicular phase,
- luteal phase.
These aren’t related to the phases of the moon.
In Fertility Awareness Based Methods, cycles are divided into fertility phases. Some methods may not use “phase” terminology at all, but instead they distinguish days simply by whether they are potentially fertile or not; a Boolean system.
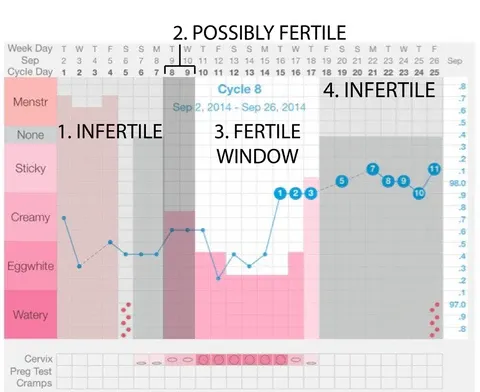
Others will use a system of three phases: Phase 1, Phase 2, and Phase 3.
- Phase 1 begins at the start of the cycle and includes the relatively infertile days prior to ovulation.
- Phase 2 are fertile days which includes days of ovulation,
- and Phase 3 encompasses the infertile days after ovulation.
Most women move through these three phases in a straightforward fashion. Others may have long or disturbed cycles, where they rotate between Phase 1 & Phase 2 before ovulation does indeed occur and they afterward enter into Phase 3.
These may overlap the biological phases, but not directly align.
Most fertility charting methods do not pinpoint ovulation to one precise day, but instead offer a window – typically between 3-5 days – of when ovulation most likely occurred.
In some methods the few days of menses may be considered potentially fertile, and in others they’re considered in Phase 1 and infertile by default. While ovulation occurs on a potentially fertile day (Phase 2), it may not be until several days after ovulation that a woman is recognized by her fertility awareness based method as being in Phase 3.
So while the biological phases and the Fertility Awareness Based Methods may differ, the end result either way is that you become a lot more knowledgeable about your cycle.
Both approaches can give you insight into your personal cycle, which you can use to any number of benefits, including monitoring your health and identifying your fertility window. And, the more you use the right lingo of course, the better conversations we'll all be able to have about our menstrual health.
If you'd like to learn more about FABM, including how to chart your cycle and identify your fertility window, download Tempdrop's free Introduction to Fertility Awareness, a beautifully-designed guide written by seven certified fertility educators.