What Is PMDD? How to Get an Accurate Diagnosis and Support
Struggling with severe premenstrual mood swings? Discover what PMDD is, how to get a proper diagnosis, and effective treatments to help you find relief.
Updated March 24, 2026

Many women are familiar with the phrase premenstrual syndrome (PMS). Just before our period our hormones drop lower and we often experience physical and emotional shifts.
However, Premenstrual Dysphoric Disorder (PMDD) is a severe, hormone-sensitive mood disorder that goes much further than typical PMS symptoms. PMDD is associated with significant distress and can severely interfere with work, school, social activities, and relationships.
Understanding the difference between the two—and what PMDD looks like in a typical cycle—is the first vital step in getting the care you deserve.
PMS vs. PMDD: What is the Difference?
Our society often makes light of PMS, which can unfortunately gaslight women into believing their extreme symptoms are just “normal.” To understand PMDD, it helps to first look at standard PMS.
Normal Premenstrual Syndrome (PMS) includes a range of mild to moderate symptoms that usually start a few days before menses. These can include:
- Mood swings or irritability
- Tender breasts and bloating
- Cramps and headaches
- Forgetfulness or trouble concentrating
- Decreased energy or feeling overwhelmed
Most people have at least some of these symptoms. While they might slow us down a bit, they shouldn’t keep us from tending to our daily tasks, and they resolve quickly during menstruation.
Premenstrual Dysphoric Disorder (PMDD), on the other hand, is estimated to affect 3–8% of the population. Officially recognized as a medical disorder in 2013, PMDD involves severe and debilitating physical and emotional symptoms that can last 1–2 weeks before menstruation. Symptoms include:
- Severe depression, anxiety, or panic attacks
- Lasting irritability, anger, or feeling out of control
- Trouble focusing and extremely low energy
- Binge eating
The impact of PMDD is profound; an estimated 15% of people with PMDD have attempted suicide. If your symptoms are severe enough that you have to miss school or work, or can’t get out of bed, this is not normal PMS, and you deserve care and intervention.
How do doctors diagnose PMDD?
Doctors base a PMDD diagnosis on a medical handbook known as the DSM-5 (Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition). The DSM-5 requires at least 5 PMDD symptoms to be present in the majority of menstrual cycles from the last year.
To fit a PMDD diagnosis, the PMDD symptoms must:
- Present in the week before the onset of menses (during the luteal phase),
- Start to improve within a few days after the onset of your period,
- And become minimal or absent in the week post-menses.
One or more of the following PMDD symptoms must be present:
- Notable affective lability (e.g., mood swings, sadness or tearfulness, or increased sensitivity to rejection).
- Notable irritability, anger, or increased interpersonal conflicts.
- Notable depressed mood, feelings of hopelessness, or self-deprecating thoughts.
- Notable anxiety, tension, and/or feelings of being ‘keyed up’ or ‘on edge’.
In addition, one (or more) of the following symptoms must be present to reach a total of five symptoms:
- Decreased interest in usual activities.
- Subjective difficulty in concentration.
- Lethargy, easy fatigability, or marked lack of energy.
- Marked change in appetite; overeating or specific food cravings.
- Hypersomnia or insomnia.
- A sense of being overwhelmed or out of control.
- Physical symptoms such as breast tenderness or swelling, joint or muscle pain, a sensation of “bloating” or weight gain.
How Tempdrop Can Help You Get a Diagnosis
If you’re concerned you may have PMDD, the best way to collect data for your doctor is by tracking your cycle and your symptoms. Keep a daily record of when your symptoms show up, what they are, and how severe they feel - you could even add a rating of your symptoms in your personal comments in the app.
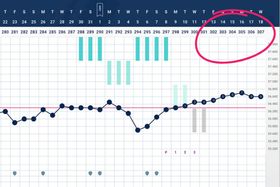
Having precise basal body temperature (BBT) data ensures that a healthcare provider has the information necessary for an accurate diagnosis. Charting your menstrual cycles also helps you learn whether your estrogen and progesterone are in balance. Without cycle tracking, it’s much more difficult to pinpoint your luteal phase (the time from ovulation to your next period) and understand if you are dealing with PMDD or a different condition. (Tip: Check out the Tempdrop Community or check in with an instructor if you need help interpreting your charts!)
How Can You Manage and Treat Symptoms?
If you are suffering from PMDD, there are ways to support your body and manage your symptoms. Note: This does not serve as medical advice. Any care plan for PMDD should be discussed with your healthcare provider.
- Diet: An anti-inflammatory diet decreases the amount of histamine our body makes, which can decrease period pain. Try steering clear of sugar, alcohol, caffeine, and gluten during the week before your period.
- Hormone Balance: Higher estrogen can cause stronger cramps and a heavier flow, as well as less stable blood sugar (which leads to cravings and mood swings!).
- Check Your Exposures: Hormone imbalances can be triggered by endocrine disruptors (or xenoestrogens) present in cosmetics, cleaning products, and pesticides. Support your body’s detox pathways by staying hydrated, supporting your liver, sweating, getting enough sleep, and having a solid stress-management plan. Be sure to check out Tempdrop’s blog about reducing endocrine disruptors.
- Supplement: Low magnesium levels can be responsible for cyclical headaches, breast pain, and cramps. Calcium helps relieve menstrual pain, and Vitamin B6 plays a vital role in creating mood-regulating neurotransmitters to mediate emotional symptoms.
- Use Your Plant Allies: A few plants to learn about include Ashwagandha, Evening Primrose Oil, Milk Thistle, Dandelion, Vitex, CBD, St. John’s Wort, Red Raspberry Leaf, and Ginkgo. Because plant medicine is complicated, it’s recommended to work with an experienced clinician who can find the right supplement and dosage for your specific symptoms.
- Medical Intervention: If your symptoms are severe, work with a healthcare practitioner to make a plan. They may suggest using DAO or progesterone therapy (progesterone up-regulates the DAO enzyme, which clears the histamine causing your symptoms). They may also suggest a Selective Serotonin Reuptake Inhibitor (SSRI). Research shows that 75% of people who tried SSRIs reported at least some relief from PMDD symptoms.
Next Steps: Remember to Listen to Your Body
The best way to figure out if you have PMDD? Start tracking your cycle and your symptoms.
Keeping a record of when in your cycle your symptoms show up, what they are, and how severe they feel gives your healthcare provider the information they need for an accurate diagnosis.
Without cycle tracking, it’s much harder to tell what’s happening — and you deserve clear answers.
Frequently Asked Questions
Is PMDD a mental illness or a hormonal imbalance?
PMDD is a diagnosable hormone-mediated mood disorder. It represents an abnormal, severe brain reaction to the normal hormonal fluctuations that happen during the menstrual cycle.
How do I know if I have PMDD or just bad PMS?
PMDD is a diagnosable hormone-mediated mood disorder. It represents an abnormal, severe brain reaction to the normal hormonal fluctuations that happen during the menstrual cycle.
Why do I feel like a different person before my period?
There are normal hormonal shifts (like the steep drop in estrogen and progesterone) that cause us to feel different during our luteal phase. However, if you are noticing extreme shifts that impact your quality of life, it is best to see a medical provider and track your cycle to determine if you may have PMDD.
Can diet and lifestyle changes help with PMDD?
Yes! Eating an anti-inflammatory diet can decrease the amount of histamine your body makes, which can help reduce period pain and symptoms. Steering clear of sugar, alcohol, caffeine, and gluten in the week leading up to your period, staying hydrated, and managing stress can all support your body in reducing severe premenstrual symptoms.
Are there natural supplements for PMDD and severe PMS?
Many people find relief through supplements and plant allies. Low magnesium levels can contribute to cyclical headaches and cramps, while Vitamin B6 plays a role in creating mood-regulating neurotransmitters. Herbs like Ashwagandha, Vitex, and Evening Primrose Oil can also offer support, though it is always recommended to work with an experienced herbalist or healthcare provider when starting plant medicine.